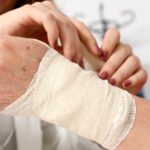
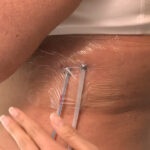
Skin maceration is a condition that’s fairly common. If you’ve ever spent a long period of time swimming or soaking in a tub, you’ve probably noticed the skin’s soft, whitish, wrinkled appearance that results.
In simplest terms, it’s oversaturated skin caused by prolonged exposure to water or moisture. In ordinary circumstances like bathing, it’s rather harmless and not a problem. When macerated skin occurs around wounds, however, you need to take steps to avoid further complications.
Key Takeaways
- Maceration Defined: Softening and whitening of skin from prolonged moisture exposure.
- Common Causes: Causes include excessive sweating, urinary incontinence, and inadequate wound care.
- Symptoms: Symptoms include pale, wrinkled skin, rashes, itching, and swelling near wounds.
- Risks: Increased risk of infection and delayed healing around wounds.
- Home Care: Basic care involves cleaning with sterile gauze, applying antiseptic creams, and using breathable bandages.
How Does It Happen?

In addition to swimming and bathing situations, maceration can also occur as a result of:
- Excessive sweating.
- Urinary incontinence.
- Wading or working in water without protective gear.
- Not changing wound dressings often enough.
- Extended bed rest, especially while recovering from surgery.
- Occlusive therapy using films or other nonbreathable, nonporous materials like latex that keep a wound dressing watertight and protected from exposure to air so as to prevent infection.
Signs of Trouble To Watch Out For

When skin maceration occurs in connection with slow-healing wounds, bed sores, ulcers, third degree burns or other health concerns, here are some symptoms to be aware of:
- A moist, spongy wound.
- Visibly wrinkled, pale white skin.
- Rash or red patches.
- Itching, burning or pain.
- Unusual swelling around the edge of a wound.
- Thick, foul smelling discharge.
If you notice any of these happening, talk to your doctor or health care professional as soon as possible, describing your symptoms so that your provider can make adjustments to your treatment plan.
How To Treat Maceration

In general, it is always important to contact your doctor if you have any questions or concerns, but here are a few at-home solutions for treating skin macerations.
- Using sterile gauze pads, clean excess fluid from the wound.
- Rinse the wound using a clean syringe filled with sterile water to remove any accumulated pus or oozing matter.
- Apply just a small amount of Bacitracin, Neosporin or a similar antiseptic/anesthetic cream or spray, covering but not smothering the wound.
- Re-cover the wound with a breathable bandage.
- Every four hours, recheck the wound, replacing the bandage and cleaning up any additional pus or ooze.
- If the condition of the wound worsens and infection develops, get medical assistance immediately.
Preventing Maceration
Many instances of skin maceration don’t require anything more than a little fresh air to dry the skin. When the skin is broken, it’s better to have air circulating around the wound rather than keeping it bandaged once a scab has formed. One precaution you’ll want to take, however, is to recover the wound to keep it germ-free if you plan to be at work or do any manual labor.
Lifestyle Adjustments to Prevent Maceration

Simple lifestyle changes can significantly reduce the risk of skin maceration:
- Hydration and Nutrition: Adequate hydration and a balanced diet support skin health and its natural moisture-regulating mechanisms.
- Mindful Bathing Practices: Limiting time spent in water and using gentle, non-drying soaps can help.
- Clothing Choices: Wearing breathable, moisture-wicking fabrics, especially during exercise, can be beneficial.
Psychological Impact of Chronic Skin Conditions
It’s important to acknowledge the psychological aspect:
- Emotional Well-being: Chronic skin conditions, including recurrent maceration, can affect one’s self-esteem and emotional health.
- Support Systems: Seeking support from dermatologists, counselors, or support groups can be essential for managing the psychological impacts.
FAQ
Can Skin Maceration Lead to Infections?
Yes, prolonged skin maceration, particularly around wounds, increases the risk of bacterial and fungal infections due to the compromised skin barrier.
Is it More Common in Certain Age Groups?
While it can occur at any age, the elderly and infants are more prone due to thinner skin and more sensitive skin barriers.
How Can I Tell if My Wound is Macerated?
Look for signs like overly white or pruney skin, a spongy texture around the wound, and increased tenderness or pain.
Are There Any Medical Conditions That Increase the Risk of Maceration?
Conditions like lymphedema, venous insufficiency, and diabetes can increase the risk due to fluid retention and reduced healing capacity.
Can It Affect Areas Other Than Wounds?
Yes, areas prone to moisture, such as under the breasts, groin, and between toes, can also experience maceration.
Should I Always Use Antiseptic Creams on a Macerated Wound?
While antiseptic creams can help, it’s essential to consult with a healthcare professional for appropriate treatment.
Can Over-the-Counter Medications Treat?
Mild cases may be managed with over-the-counter products, but persistent or severe cases require professional medical advice.
Final Words
Remember, while skin maceration is often a minor issue, its occurrence around wounds demands attention. Early intervention and proper care can prevent complications. Always consult a healthcare professional for personalized advice, especially in chronic or severe cases. Your skin health is an integral part of your overall well-being, so take steps to protect and nurture it.