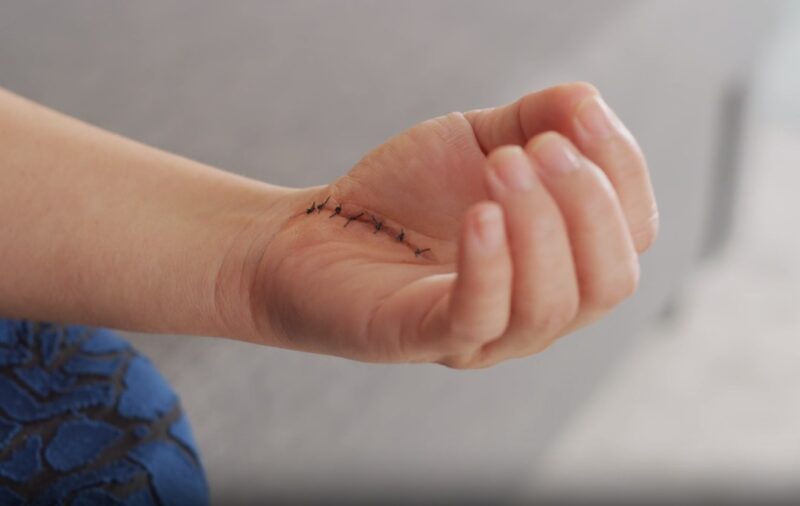
Colors play a crucial role in our lives, serving as cues and warnings in various contexts. This principle applies equally to monitoring wound healing.
The hues and tones of a wound can provide vital insights into its healing stage, indicating whether the condition is improving or worsening.
Let’s explore the different colors associated with wound healing and their meanings.
The color of a wound can tell you a lot about the progress of treatment. Color is often used as a signal and to issue.
Key Takeaways
- Red wounds signify healthy granulation tissue, crucial for wound repair, but require protection and regular monitoring for infection or complications.
- Yellow wounds indicate potential infection or inflammation and necessitate immediate clinical attention and specific cleaning methods like hydrotherapy.
- Black wounds, showing necrosis due to insufficient blood supply, require urgent medical attention, typically involving debridement and moist dressing application.
Red Wounds
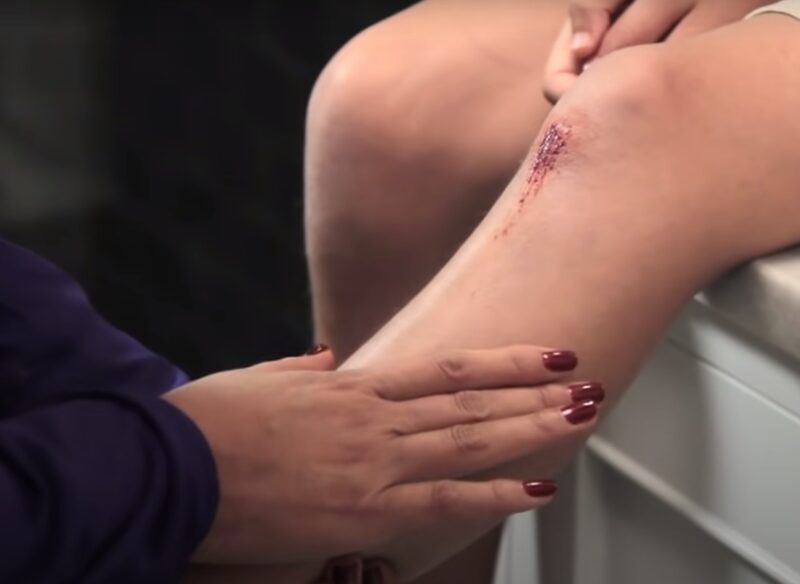
The red coloration is primarily due to the formation of granulation tissue, a critical phase in wound repair. This tissue, initially pinkish in hue, gradually deepens to a robust red or a shade reminiscent of red grapefruit as it thickens and matures.
It’s composed of new connective tissue and tiny blood vessels that form on the surface of a wound during the healing process. It is also crucial to learn how to recognize whether the healing process is active or not.
Granulation tissue plays a key role in repairing the wound from the inside out, filling the wound space with new tissue and providing a necessary foundation for the growth of skin cells.
Its rich blood supply is what gives it the characteristic red color, indicating a healthy blood flow essential for delivering nutrients and oxygen that aid in healing.
Managing Exudate
As the granulation tissue develops, it’s common for a clear fluid, known as exudate, to seep from the wound. This fluid is part of the body’s natural response to injury and plays a crucial role in the healing process.
It helps to keep the wound clean by flushing out dead cells and debris, and its presence is generally a sign of active healing. However, excessive exudate can be a concern and should be monitored.
Importance of Protecting Red Wounds

While red wounds indicate a positive healing trajectory, they can be tender and susceptible to infection. Therefore, protecting the wound is a paramount concern at this stage.
Covering the wound with a gauze bandage is recommended. The bandage should be soaked in sterile saline, which helps to maintain a moist environment conducive to healing.
Alternatively, bandages coated with antibiotics can be used to reduce the risk of bacterial infection. It’s important to change the dressings regularly to prevent infection and to assess the wound’s progress.
Care should be taken to handle the wound gently, as the new granulation tissue can be fragile.
Monitoring for Complications
Despite being a positive sign, red wounds still require careful monitoring. Any changes in the color, size, or amount of exudate, as well as increasing pain or foul odor, should be promptly addressed. These could be indicators of complications such as infection or insufficient healing.
According to Alyssa Smolen from OSF Healthcare: “How long it takes for a cut to heal can vary depending on the wound. If you notice your cut isn’t healing within a month, it’s considered a chronic wound and it’s time to talk to a wound care specialist.”
Yellow Wounds
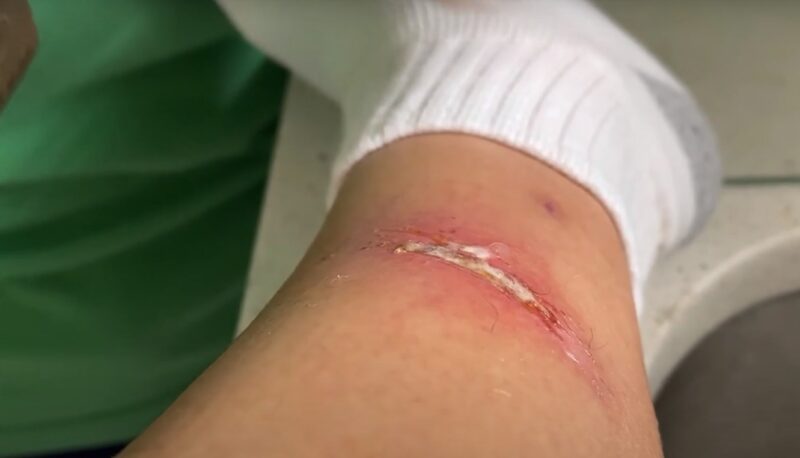
When a wound displays a yellow color, it typically points to the presence of exudate, a condition often linked with an accumulation of microorganisms. In such scenarios, the body’s immune system might be overwhelmed and unable to effectively combat these germs.
The yellow tint is a result of an excess of protein and cellular debris, which is a byproduct of the body’s response to infection or inflammation.
The Significance of Exudate
Exudate is essentially a fluid that leaks out of blood vessels into the surrounding tissues as a response to inflammation.
While a small amount of exudate can be beneficial for wound healing, providing nutrients and immune cells to the area, excessive exudate can create an environment conducive to bacterial growth.
This can hinder the healing process and potentially lead to wound infection.
Immediate Clinical Attention
A wound that turns yellow should be promptly evaluated by a healthcare professional. This color change can indicate a stalled healing process and a potential infection that needs to be addressed. Timely intervention is crucial to prevent the condition from worsening.
Effective Cleaning Methods
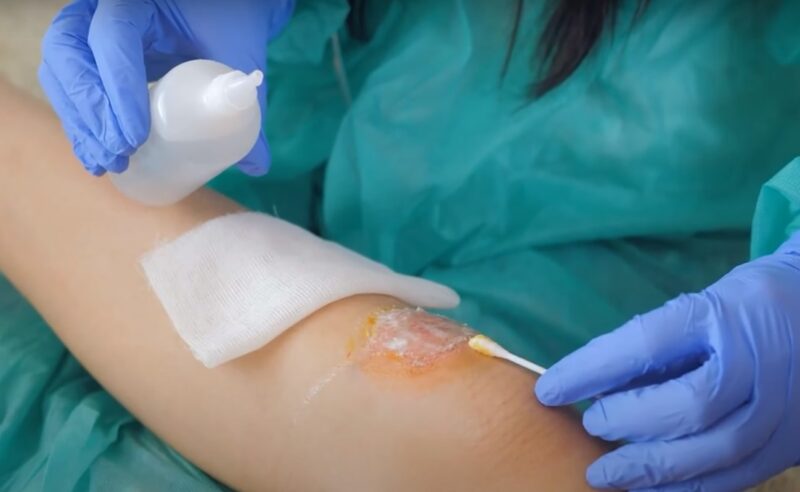
To manage yellow wounds, effective cleaning methods are essential. Techniques such as hydrotherapy or high-pressure irrigation can be employed to cleanse the wound.
These methods help in removing the exudate, debris, and any accumulated bacteria, thereby reducing the risk of infection and facilitating the healing process. Hydrotherapy uses water to gently clean and stimulate the wound area, promoting blood flow and healing.
High-pressure irrigation, on the other hand, employs a more forceful stream of saline or other solutions to thoroughly clean the wound, dislodging and removing exudate and debris.
Application of Moist Wound Bandages
After cleaning, it’s important to cover the wound with a moist wound bandage. These bandages help maintain a moist environment, which is essential for wound healing.
They also protect the wound from external contaminants, reduce the risk of infection, and prevent the wound from drying out, which can delay healing.
Mixed Colors

The presence of both colors indicates a mixed condition within the wound environment. The red aspect signifies healthy granulation tissue, indicative of normal healing, while the yellow coloration can point to the presence of exudate and possible microbial invasion.
This blend of colors represents a wound that is partially healing but also facing potential complications. Such a scenario requires a nuanced approach to treatment and management.
Prioritizing Treatment Based on Color
To treat wounds with both red and yellow tissue, focus on the yellow parts first. Yellow tissue may mean infection or slow healing, which can harm the whole wound.
This approach is adopted because the potential risks associated with the yellow areas, such as infection or delayed healing, can undermine the overall healing process.
The Need for Professional Assessment
When encountering a mixed-color wound, consulting with a healthcare professional becomes essential. A clinician can accurately assess the wound, considering factors such as the extent of each color, the wound’s overall condition, and any signs of infection or other complications.
This assessment is critical to formulating an effective treatment strategy. Contacting the professionals is the only way to avoid mistakes that could lead to serious side-effects. The treatment is not the same for burns, cuts, and other injuries.
Proper Treatment
The treatment of mixed-color wounds often involves a combination of strategies aimed at both fostering the healthy red granulation tissue and addressing the concerns raised by the yellow areas. This might include:
- Regular Cleaning and Debridement: To manage the exudate and potential microbial presence, regular cleaning and possibly debridement are necessary. This helps in removing unhealthy tissue and contaminants, thereby reducing the risk of infection.
- Appropriate Dressings: The choice of wound dressing is pivotal. Dressings that can manage exudate while maintaining a moist environment for the red areas are often selected. These dressings might need to have antimicrobial properties or be changed more frequently to effectively manage the mixed wound environment.
- Monitoring and Adjustments: Regular monitoring of the wound is crucial. The treatment plan may need adjustments based on how the wound responds to initial interventions.
Black Wounds and Necrosis
When a wound turns black, it’s a sign of necrosis – the death of tissue cells. Necrosis typically occurs when the blood supply to the wound area is insufficient, starving the tissue of necessary nutrients and oxygen.
This lack of blood flow not only halts the healing process but also makes the wound susceptible to further complications, including a heightened risk of serious infections. The black color in a wound is due to the accumulation of dead cells.
These cells, having lost their vitality, become a barrier to the natural healing process. The presence of dead tissue can also be a breeding ground for harmful bacteria, exacerbating the risk of infection and potentially leading to more severe health issues.
Prompt Action is Essential
When necrosis is identified, it’s imperative to seek immediate medical attention. Delaying treatment can lead to the spread of necrosis and increase the likelihood of systemic infection, which can be life-threatening.
Health professionals often employ a range of diagnostic tools to assess the extent of necrosis and formulate an appropriate treatment plan.
Effective Treatment
Debridement – The First Step
The primary treatment for a necrotic wound is debridement. This process involves the careful removal of all dead tissue from the wound area.
Debridement can be done using various methods, including surgical removal, enzymatic debridement (using specific enzymes to dissolve dead tissue), or autolytic debridement (encouraging the body’s own enzymes to break down the dead tissue).
The choice of method depends on the wound’s severity, the patient’s overall health, and other factors.
Applying a Moist Dressing

After debridement, it’s crucial to apply a moist dressing to the wound. Moist wound environments are known to facilitate healing by keeping new tissue healthy and preventing the wound from drying out.
These dressings also help in absorbing any drainage, keeping the wound clean, and protecting it from external contaminants.
Ongoing Monitoring and Care
Regular monitoring of the wound post-debridement is vital. Healthcare providers will assess the wound’s healing progress, watch for signs of infection, and make adjustments to the treatment plan as necessary.
It’s also essential for patients to follow their healthcare provider’s instructions regarding wound care at home, which may include changing dressings regularly and maintaining good hygiene around the wound area.
Comprehensive Treatment Approach
In some cases, additional treatments such as antibiotic therapy or hyperbaric oxygen therapy might be recommended. These therapies aim to improve blood flow, reduce the risk of infection, and support overall wound healing.
FAQs
Do wounds hurt while healing?
Wounds may hurt while healing because of the inflammation and nerve stimulation that occur during the healing process. The pain usually decreases as the wound heals, but some wounds may be more sensitive than others.
Will purple scars turn white?
Purple scars are usually new scars that have not fully matured yet. They may turn white over time as the blood vessels in the scar tissue shrink and the collagen fibers become more organized. This process can take months or years, depending on the type and size of the scar.
Do purple scars go away?
Purple scars may fade or become less noticeable over time, but they usually do not go away completely. Some treatments, such as silicone gel sheets, massage, sunscreen, or laser therapy, may help improve the appearance of scars. However, there is no guarantee that any treatment will make a scar disappear.
Do wounds heal faster covered or uncovered?
Wounds heal faster when they are covered with a moist dressing that prevents infection and keeps the wound environment optimal for healing. Uncovered wounds may dry out, form scabs, and delay healing. They may also be more prone to infection and scarring.
Summary
The colors of wounds are like a language, conveying crucial information about the healing process. Red wounds, with their vibrant granulation tissue, are like the green light signaling progress, yet they demand vigilant care to guard against infection.
Yellow wounds are like caution signs, hinting at possible infection or inflammation, calling for immediate medical attention. And black wounds? They are the red flags of necrosis, urging swift and decisive action to prevent severe complications.